When Joint Degeneration Becomes a Life-Limiting Condition
Osteoarthritis of the hip and knee is one of the most prevalent and disabling musculoskeletal conditions worldwide. Far from being a benign consequence of aging, hip and knee osteoarthritis represent a major public health and socioeconomic challenge, profoundly affecting mobility, independence, productivity, and quality of life. As populations age and life expectancy increases, the burden of joint degeneration continues to rise, placing unprecedented pressure on healthcare systems, societies, and individuals.
Osteoarthritis is now increasingly recognized as a whole-joint disease rather than an isolated cartilage disorder. In addition to cartilage degeneration, osteoarthritis involves pathological changes in subchondral bone, synovium, ligaments, menisci (in the knee), and periarticular muscles. This complex, multi-tissue involvement helps explain the progressive nature of the disease and the variability in symptoms and clinical outcomes among patients with similar radiographic findings.
Despite advances in conservative treatments, many patients eventually progress to end-stage disease, where pain and functional limitations often require joint replacement surgery. Hip and knee arthroplasty are among the most successful procedures in modern medicine, yet they are not without limitations. A substantial proportion of patients remain partially dissatisfied; complications still occur, and current “one-size-fits-all” implant solutions fail to accommodate the wide anatomical variability of human joints.
In this context, emerging technologies for patient-specific implant designs using Additive Manufacturing (AM) offer a transformative opportunity to rethink how orthopedic implants are designed, manufactured, and delivered.
The Epidemiology of Hip and Knee Osteoarthritis: A Silent Epidemic
Osteoarthritis is the most common form of arthritis and a leading cause of disability globally. The hip and knee are among the most frequently affected joints due to their load-bearing function and exposure to repetitive mechanical stress.
Epidemiological data indicate that:
- In 2020, 595 million people worldwide had osteoarthritis, equivalent to approximately 7.6% of the global population — an increase of +132% since 1990.
- Knee osteoarthritis affects hundreds of millions of individuals worldwide.
- Hip osteoarthritis, although less prevalent than knee OA, often results in more severe functional impairment.
- The lifetime risk of developing symptomatic knee OA can exceed 40%, while hip OA affects up to 25% of individuals in certain populations. Knee osteoarthritis, due to its higher and increasing prevalence, is of major concern.
- The age-standardized rate of YLDs per 100,000 varies across Europe, with Eastern Europe recording the highest burden at 294.6, compared to 264.5 in Western Europe, 257.4 in Central Europe, and an average of 255.0 worldwide.
By 2050, cases of hip and knee osteoarthritis are projected to increase significantly, with an expected rise of 78.6% and 74.9%, respectively (GBD 2021 Osteoarthritis Collaborators, 2023).
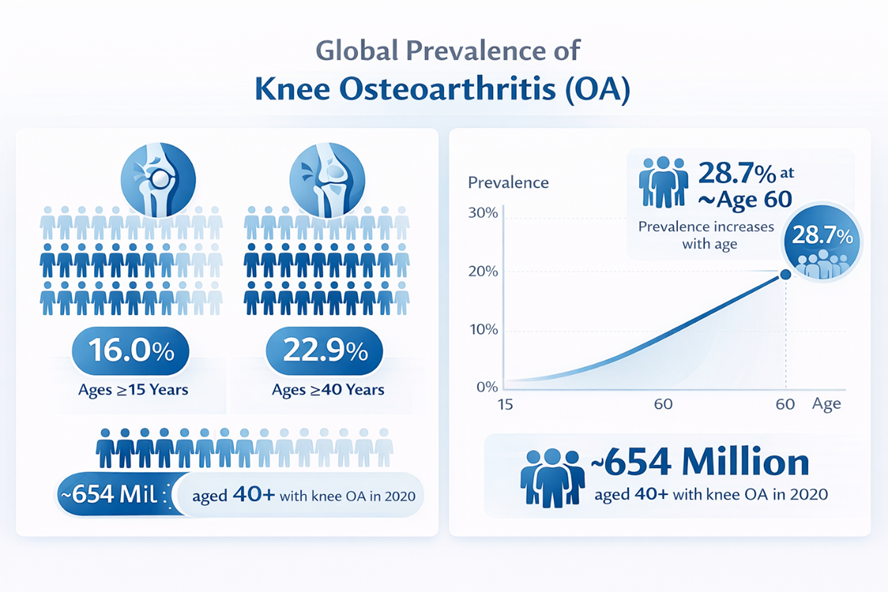
Figure 1 – The global prevalence of knee osteoarthritis is estimated at 16.0% among adults aged 15 and over, rising to 22.9% in individuals aged 40 and above, corresponding to an estimated 654 million people worldwide in 2020. Prevalence increases with age, reaching approximately 28.7% around 60 years of age. Data from large pooled meta‑analyses of population‑based studies (Cui et al., 2020).
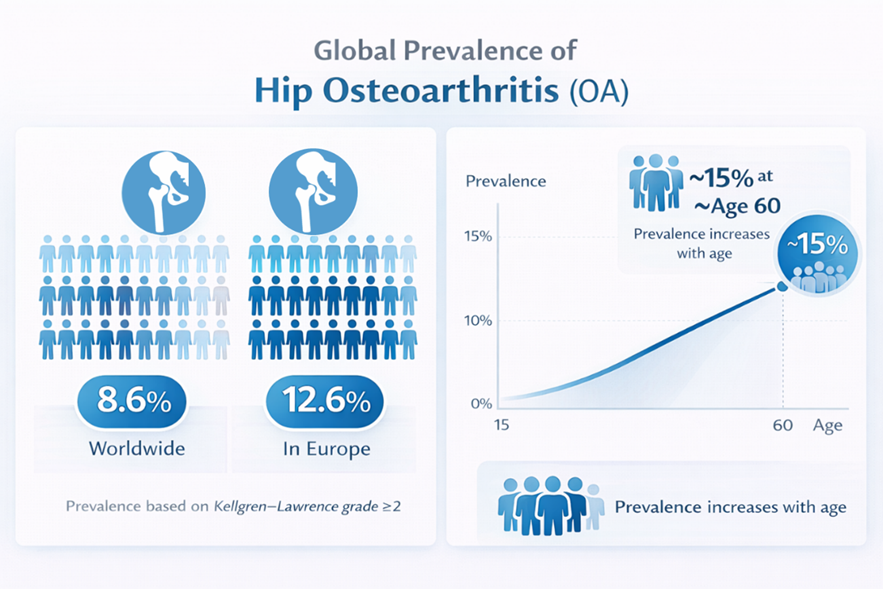
Figure 2 – Global radiographic prevalence of hip osteoarthritis is estimated at 8.6% worldwide, with the highest regional prevalence reported in Europe at 12.6% (Kellgren–Lawrence grade ≥2). Hip osteoarthritis prevalence increases with age but does not differ significantly by sex. These values are based on meta‑analysis of over 30 population studies (Fan et al., 2023).
The increasing incidence of OA is strongly associated with:
- Aging populations
- Increased life expectancy
- Rising obesity rates
- Higher participation in sports and physically demanding activities
- Traumatic joint injuries, including those related to traffic accidents
Together, these factors contribute to a continuously expanding pool of patients who will eventually require advanced orthopedic care.
Importantly, osteoarthritis remains significantly underdiagnosed in its early stages, while disease progression is often nonlinear and patient-specific. Structural joint damage may advance even when symptoms appear mild, delaying appropriate intervention and contributing to worse outcomes at later stages.
Functional Limitations and Impact on Daily Life: More Than Just Joint Pain
Hip and knee osteoarthritis progressively impair joint biomechanics, leading to pain, stiffness, instability, and loss of range of motion. These symptoms directly translate into functional limitations that affect nearly every aspect of daily living.
Common patient-reported limitations include:
- Difficulty walking, climbing stairs, or standing for prolonged periods
- Reduced ability to perform self-care activities
- Loss of independence and increased reliance on caregivers
- Decreased participation in work, sports, and social activities
- Sleep disturbances due to chronic pain
Beyond physical impairment, osteoarthritis has a profound psychological impact, often associated with anxiety, depression, and social isolation. The cumulative effect is a substantial reduction in health-related quality of life, comparable to that seen in chronic cardiovascular or neurological diseases.
Notably, the severity of pain and functional impairment does not always correlate with radiographic disease severity. Some patients experience substantial disability with relatively modest structural changes, while others remain functional despite advanced joint degeneration. This dissociation highlights the multifactorial nature of osteoarthritis-related disability and reinforces the need for patient-centered evaluation and treatment strategies.
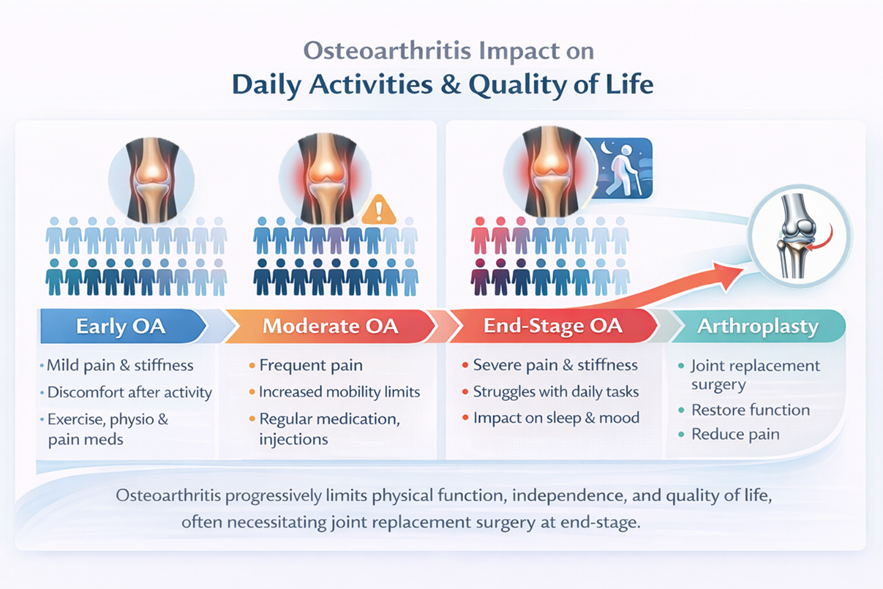
Figure 3 – Osteoarthritis progressively limits physical function, independence, and quality of life. Early disease often responds to conservative measures, but many patients eventually progress to end-stage disease, where joint replacement becomes necessary to restore function and reduce pain.
Socio-Economic Implications of Osteoarthritis: A Growing Burden on Healthcare Systems and Society
The socio-economic impact of hip and knee osteoarthritis extends far beyond the individual patient. Osteoarthritis is one of the leading causes of years lived with disability (YLDs) globally and represents a major driver of healthcare expenditure.
Key socio-economic consequences include:
- Direct healthcare costs, including outpatient visits, imaging, medications, physiotherapy, and surgical interventions.
- Indirect costs due to work absenteeism, reduced productivity, early retirement, and disability pensions
- Caregiver burden, particularly in advanced disease stages
- Inequalities in access to care, especially in low- and middle-income regions
As demand for joint arthroplasty continues to rise, healthcare systems face increasing pressure to deliver effective, durable, and cost-efficient solutions without compromising patient outcomes.
Conservative Treatment: Necessary But Often Insufficient: Slowing Progression, Not Reversing Disease
Initial management of hip and knee osteoarthritis focuses on non-surgical strategies, including:
- Patient education and lifestyle modification
- Weight management
- Physical therapy and exercise programs
- Pharmacological pain management
- Intra-articular injections
While these management approaches are essential for symptom control and delaying disease progression, they do not reverse structural joint damage. As osteoarthritis progresses toward joint failure, the biological and biomechanical environment becomes increasingly unfavorable, limiting the long-term effectiveness of non-surgical interventions. For many patients, conservative treatment eventually becomes insufficient, particularly in advanced stages characterized by severe cartilage loss, deformity, and bone remodeling. At this point, joint replacement surgery often represents the only viable option to restore function and alleviate pain.
Hip and Knee Arthroplasty: A Cornerstone of Modern Orthopedics: Scale and Clinical Success
Hip and knee replacements are among the most commonly performed surgical procedures worldwide. In Europe, global estimates point to:
- Over 3.1 million hip replacements
- More than 2.5 million knee replacements
However, these figures are underestimated and the true prevalence is expected to be increasingly higher. Moreover, the arthroplasty demand is expected to increase by over 37% by 2060 (Lübbeke et al., 2018).
From a clinical standpoint, joint arthroplasty delivers:
- Significant pain relief
- Improved mobility and function
- Overall improvement in quality of life
These procedures have transformed the lives of millions of patients and remain a cornerstone of orthopedic care.
However, clinical success defined by implant survival does not always translate into patient-perceived success. Patient-reported outcome measures (PROMs) have revealed that a substantial proportion of individuals, particularly after knee arthroplasty, continue to experience residual pain, functional limitations, or dissatisfaction, despite technically successful procedures.
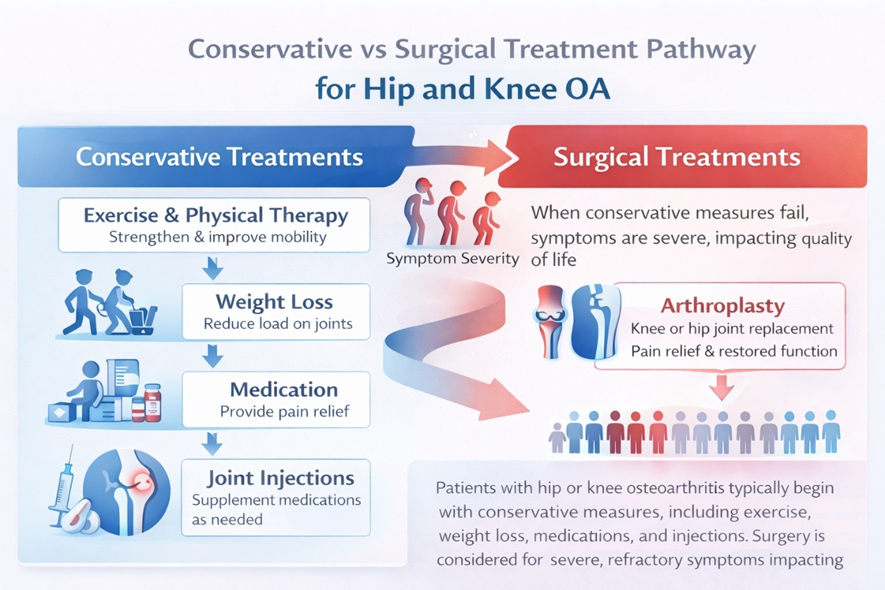
Figure 4 – Conservative vs surgical treatment pathway for hip and knee osteoarthritis.
Limitations and Complications of Conventional Implants: Why Current Solutions Are Not Enough
Despite their success, standard hip and knee implants are associated with several limitations:
Anatomical Mismatch
Conventional implants are produced in standardized sizes, requiring surgeons to select the “closest fit” from a predefined inventory. However, human joint anatomy varies widely in shape, size, and morphology, often leading to:
- Prosthetic over- or under-coverage
- Suboptimal bone-implant contact
- Altered joint biomechanics
Patient Dissatisfaction
A notable proportion of patients, particularly after knee arthroplasty, report persistent pain, stiffness, or functional limitations despite technically successful surgery. This dissatisfaction is multifactorial and has been linked not only to surgical factors, but also to individual anatomy, joint kinematics, soft-tissue balance, and patient expectations. Standardized implant designs may fail to adequately reproduce native joint biomechanics, particularly in anatomically diverse populations.
Surgical and Post-Operative Complications
There are several complications that may arise after a joint arthroplasty, which may include:
- Implant loosening
- Wear debris and osteolysis
- Periprosthetic fractures
- Infection
- Need for revision surgery
Even relatively low complication rates translate into a substantial absolute number of affected patients given the scale of joint replacement procedures.
The Need for a Paradigm Shift in Orthopedic Implant Design: From Standardization to Personalization
Given the recognized heterogeneity of osteoarthritis – encompassing different mechanical, biological, and inflammatory phenotypes – it is increasingly clear that standardized implant solutions may not optimally serve all patients. A paradigm shift toward personalization is therefore not only technological, but also biological and clinical.
The limitations of conventional implants highlight a fundamental issue: current manufacturing and design paradigms are not fully aligned with patient-specific anatomy and biomechanics.
An ideal implant should:
- Match the patient’s unique joint morphology
- Optimize load distribution and joint kinematics
- Promote stable bone integration
- Reduce complication and revision rates
Achieving these goals with traditional manufacturing techniques remains challenging.
Personalized Orthopedic Implants: Addressing Unmet Clinical Needs and Why Patient-Specific Solutions Matter
Personalized implants are designed based on individual anatomy derived from medical imaging, such as computed tomography (CT) or magnetic resonance imaging (MRI) scans. Additive manufacturing, commonly referred to as 3D printing, represents a major technological leap in orthopedic implant production. Additive manufacturing is particularly well suited for metallic orthopedic implants, where structural integrity, fatigue resistance, and biological performance are critical. Unlike subtractive manufacturing, additive manufacturing enables the fabrication of complex geometries layer by layer, offering unprecedented design freedom.
By tailoring implant geometry to the patient, these solutions can:
- Optimize bone-implant fit (the implant fits the patient and not the patient to the implant)
- Improve joint alignment and biomechanics
- Reduce the risk of implant malposition
- Potentially shorten surgical time
- Reduce the risk of complications and revision related to implant malposition and loosening
Importantly, personalized implants address one of the main sources of dissatisfaction in joint arthroplasty: the mismatch between standardized components and individual joint morphology. Beyond geometric matching, patient-specific implants enable a shift toward function-driven design, where implant geometry, fixation strategy, and surface architecture are optimized to better replicate native joint biomechanics and load transfer. This approach holds particular promise in addressing persistent dissatisfaction and improving long-term functional outcomes.
The Future of Hip and Knee Arthroplasty: A Patient-Centered Vision
As the prevalence of osteoarthritis continues to rise, the future of joint replacement will increasingly depend on:
- Personalized implant solutions
- Intelligent manufacturing technologies
- Sustainable production models
- Data-driven design and validation
These advances have the potential not only to improve clinical outcomes but also to redefine how orthopedic care is delivered—placing the patient at the center of innovation.
Rethinking Joint Replacement for a Growing Global Need
Hip and knee osteoarthritis represent a major and growing challenge for individuals and healthcare systems alike. While joint replacement surgery remains an effective solution for advanced disease, current implant technologies fall short of fully addressing patient-specific needs.
Recognizing osteoarthritis as a heterogeneous, whole-joint disease underscores the limitations of standardized solutions and strengthens the rationale for patient-specific approaches. In this evolving landscape, personalized implants manufactured through advanced additive manufacturing technologies represent a critical step toward more functional, durable, and patient-aligned joint replacement solutions.
Additive manufacturing and personalized implant design offer a compelling pathway toward more precise, effective, and sustainable orthopedic solutions. By embracing these technologies, the orthopedic community can move beyond standardized approaches and toward a future where implants are designed not just for joints—but for people.
Keep following our blog posts for more updates and developements at: https://www.adapt-smart.eu/blog/


